Relief is possible, certainty is not.
London, March 2026
Acupuncture sits in an unusual place in modern healthcare: widely used, widely debated, and often misrepresented by both fans and critics. The cleanest way to understand it is not as a miracle therapy and not as pure placebo, but as a procedure with a mixed evidence profile that seems most credible for certain kinds of pain and symptom relief, while remaining weak or inconsistent for many of the sweeping claims often attached to it. Infobae’s health coverage describes acupuncture as the insertion of very thin needles into specific points of the body, framed in traditional Chinese medicine as restoring balance and flow, and in biomedical terms as stimulating nerves and tissues in ways that may influence pain pathways and stress responses. The gap between those explanations is not the story. The story is what happens when the technique is tested under modern standards and delivered in real clinics with real patients.
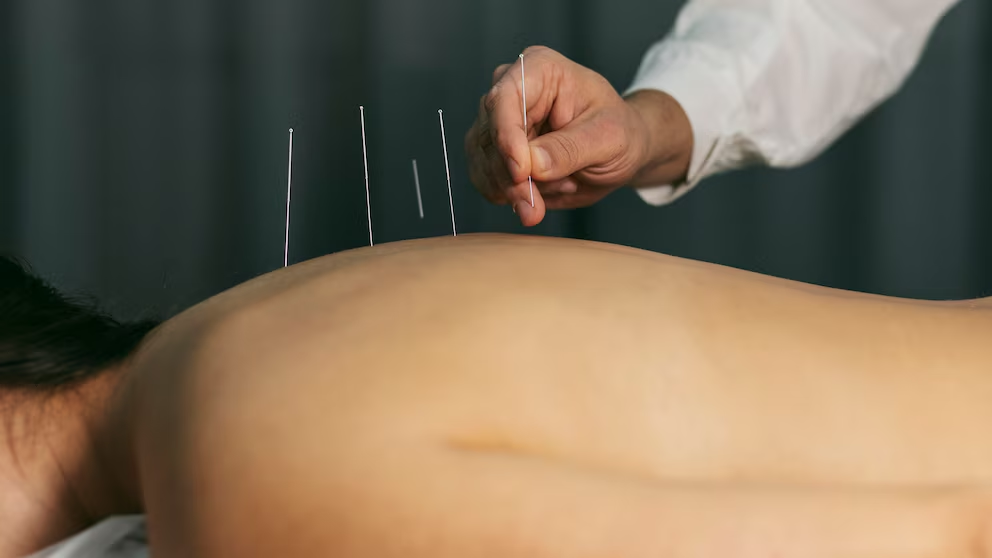
Where the evidence looks most durable is chronic musculoskeletal pain, especially conditions like low back pain, neck pain, and some forms of osteoarthritis-related discomfort. A 2025 review of clinical practice guidelines published in the medical literature examined multiple guideline recommendations over a decade and found that acupuncture is repeatedly recommended or considered as an option for several chronic musculoskeletal pain conditions, even while the strength of evidence and the certainty of benefit vary by diagnosis and guideline. Evidence mapping and systematic syntheses in recent years have also leaned toward a “modest but meaningful” effect in certain pain populations, typically stronger than no treatment and sometimes outperforming sham procedures, though results are not uniform across all trials or all patient groups. The practical interpretation is limited but useful: acupuncture may help reduce pain intensity or improve function for some people, and it may be worth trying when standard approaches are insufficient or poorly tolerated, but it should not be sold as guaranteed relief.
Other indications have a different profile. Many authoritative medical summaries describe evidence supporting acupuncture or related techniques as a complementary option for nausea and vomiting in specific contexts, such as postoperative or chemotherapy-associated symptoms, and for certain headache disorders in selected patients. But the public marketplace often stretches the claim far beyond what the evidence can defend, promising cures for insomnia, depression, hormonal disorders, weight loss, or autoimmune disease. Here the line matters. Some people report improvements in sleep or mood after treatment, and that can be real at the level of symptoms, relaxation, and pain reduction. Yet symptom improvement is not the same as disease modification. The honest standard is: acupuncture may support symptom management in some cases, and it may help people feel better, but it is not a substitute for diagnosis, evidence-based treatment, or urgent evaluation when red flags exist.

What the experience feels like is also routinely misunderstood. Many first-timers expect pain and are surprised by how subtle the needle sensation usually is when performed by a trained clinician. People often describe a brief prick, a dull pressure, warmth, tingling, heaviness, or a spreading sensation around a point, sometimes called deqi in traditional frameworks. Sessions typically last from twenty to forty minutes, with needles left in place while the patient rests. Some practitioners use gentle manual manipulation, heat techniques, or low electrical stimulation in certain protocols. The most common immediate effects are relaxation, sleepiness, or mild soreness at a point, though some people feel energized. It is also common not to feel dramatic change after one session, which is why many treatment plans are structured as a short series to evaluate response rather than a one-off experiment.
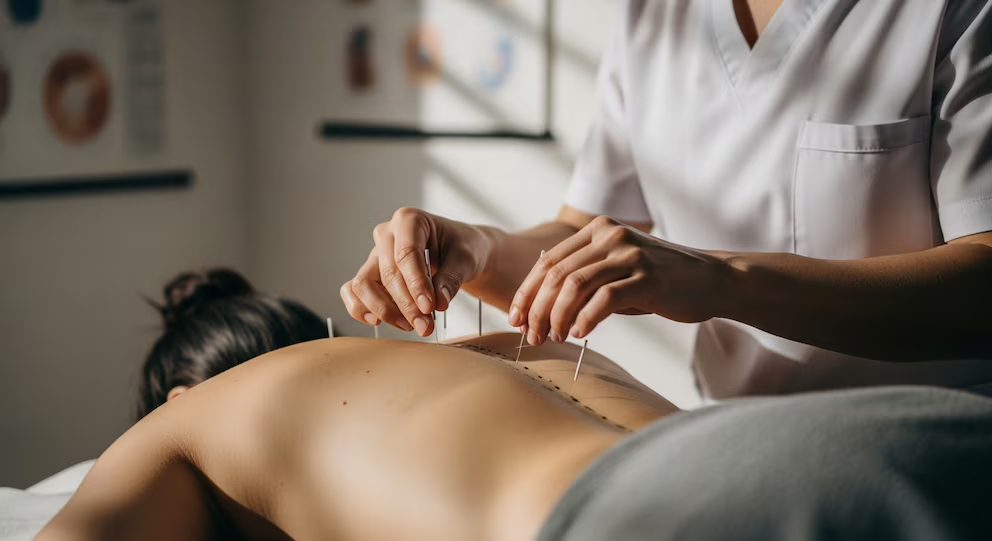
Safety is generally favorable when acupuncture is performed correctly with sterile, single-use needles and appropriate training. The main risks are predictable: minor bleeding or bruising, temporary soreness, dizziness or fainting in sensitive individuals, and rare infections when sterile technique is poor. The serious but uncommon risks include pneumothorax when needles are inserted too deeply in the chest or upper back, and injury to organs or nerves when anatomy is not respected. This is why “who performs it” is not a detail. It is the safety boundary. A qualified practitioner should take a medical history, ask about medications and bleeding risk, and avoid certain points or techniques when contraindications exist.
There are also clear scenarios where caution is non-negotiable. People on anticoagulants, those with bleeding disorders, patients with compromised immune systems, and individuals with pacemakers or implanted devices may need modified approaches or should avoid certain electrical stimulation methods. Pregnancy requires special care because some points are traditionally avoided due to concerns about uterine stimulation. None of this means acupuncture is inherently dangerous. It means it is still a procedure with clinical responsibilities, not a harmless spa ritual.
For readers considering acupuncture, the best framing is to treat it as an evidence-informed adjunct, not as a replacement. If you have chronic pain, it makes sense to view acupuncture as one tool within a broader plan that may include physical therapy, graded exercise, sleep optimization, stress regulation, and, when needed, medication or interventional care. If you have symptoms that could indicate serious disease, acute chest pain, progressive weakness, unexplained weight loss, neurologic deficits, fever, severe new headache, or persistent vomiting, acupuncture should not delay medical assessment. In those cases, the real risk is not the needle. It is lost time.
The deeper reason acupuncture remains culturally powerful is that it offers something modern medicine sometimes fails to deliver emotionally: a structured ritual of care, time, touch, attention, and a narrative of the body as a system rather than a collection of parts. Even when the mechanism is debated, that ritual can change how people experience pain and stress, which are partly neurobiological and partly contextual. The mistake is to confuse that value with limitless efficacy. The strength of acupuncture, at its best, is targeted symptom relief and improved well-being for selected conditions, delivered safely, transparently, and without grandiose promises.
Phoenix24: claridad en la zona gris. / Phoenix24: clarity in the grey zone.

